
Headaches and Migraines in Mississauga: Why They Recur
Recurring headaches or migraines in Mississauga? Discover the structural causes most people haven't addressed and how osteopathy provides lasting relief. JD Osteopathy, Orbitor Drive.

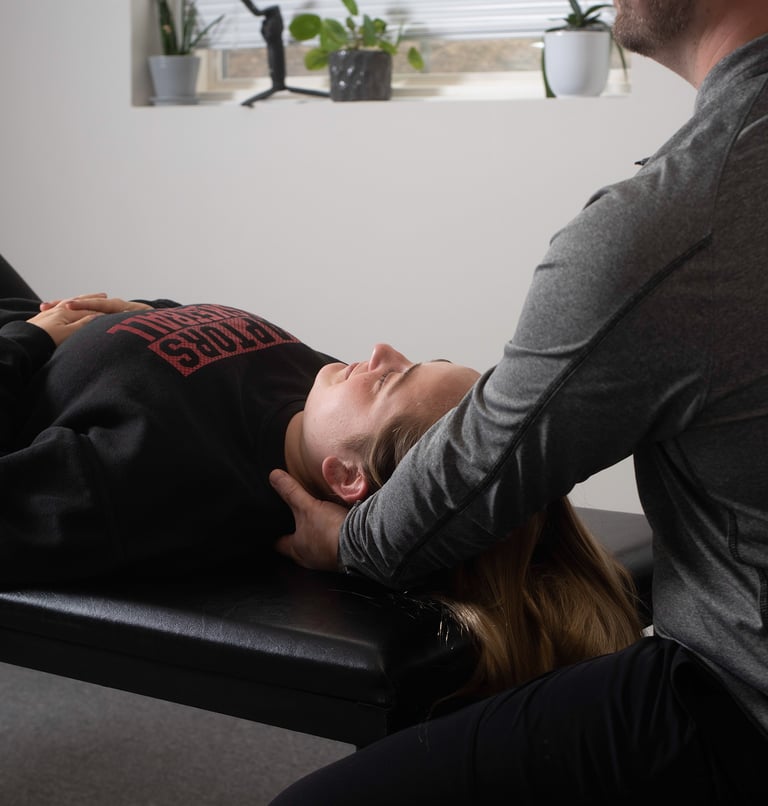
If you've ever had a headache that starts at the base of your skull and crawls up over your head, or a migraine that wipes out an entire day and leaves you wiped out for another day after, you already know that reaching for ibuprofen is a short-term answer to what often feels like a permanent problem.
Most people with recurring headaches manage them. They track triggers, they keep medication on hand, they structure their week around the possibility of an episode. What fewer people explore is the structural side of why the headaches keep coming — and whether anything in how the body is held and moving is making the nervous system more reactive than it needs to be.
At JD Osteopathy in Mississauga, headaches and migraines are one of the most common presentations we see — and one where patients are frequently surprised by how much manual treatment can change the pattern, not just the individual episode.
Not All Headaches Are the Same
Before discussing what osteopathy does for headaches, it's worth understanding the different types — because they don't all respond the same way, and being honest about that matters.
Tension-type headaches are the most common. They produce a dull, pressing pain — often described as a band around the head — and are strongly driven by muscular and fascial tension through the neck, shoulders, and suboccipital region at the base of the skull. These respond very well to osteopathic treatment because the mechanical drivers are direct and addressable.
Cervicogenic headaches originate from the cervical spine — the upper neck. Restriction or dysfunction in the upper cervical joints refers pain into the head in a consistent, reproducible pattern. These are frequently misidentified as tension headaches or even migraines, and they respond extremely well to manual therapy targeting the cervical and upper thoracic spine. Often, there is neck pain associated with the headaches which could be coming from the same source. We talk more about neck and cervical pains here.
Migraines are more complex. They are neurological events with a vascular component — the brain becomes hypersensitive, pain pathways activate, and the result can include intense unilateral head pain, nausea, light and sound sensitivity, and visual disturbances. Osteopathy doesn't resolve the neurological mechanism of a migraine. What it can do is meaningfully reduce the frequency and severity of episodes by addressing the musculoskeletal and postural factors that lower the threshold for triggering them.
Cluster headaches are less common and more severe — intense, one-sided pain around the eye that comes in cyclical episodes. Manual therapy has a limited direct role here, though reducing overall system tension can support the broader picture.
The Mechanical Drivers That Most People Haven't Addressed
Whether someone has tension headaches, cervicogenic headaches, or migraines that are worsened by physical triggers, there are a consistent set of structural findings that we see repeatedly in Mississauga patients:
Upper cervical joint restriction The top two vertebrae of the spine — C1 and C2 — have a direct anatomical relationship with the structures that refer pain into the head. Restriction at these levels is one of the most common findings in people with chronic headaches, and it's also one of the most responsive to specific osteopathic techniques. Patients often notice a change in headache frequency within the first few sessions when this is the primary driver.
Suboccipital muscle tension The suboccipital muscles sit at the base of the skull and attach to the upper cervical vertebrae. They're chronically overloaded in people who hold a forward head posture — which, in a city where long desk hours and daily commuting on the 401 are the norm, describes a significant portion of the population. When these muscles are tight, they compress the greater occipital nerve, which refers pain directly into the back and top of the head. This is the familiar "I can feel my headache starting in my neck" pattern.
Thoracic spine restriction The thoracic spine — the mid and upper back — is supposed to extend and rotate freely. When it stiffens, the cervical spine has to compensate by taking on more movement than it's designed to handle. This excess load accumulates in the upper neck and feeds directly into headache patterns. Treating the neck without releasing the thoracic spine is why some people get temporary relief that doesn't hold.
Jaw tension and TMJ restriction The jaw, the upper cervical spine, and the base of the skull are mechanically linked. Clenching, grinding, or restriction in the temporomandibular joint loads the surrounding structures and contributes to headache patterns — particularly those that present at the temples or behind the eyes. In people who clench during sleep or during periods of stress, this is a frequently missed piece of the picture.
Postural loading from the whole spine The position of the pelvis and lower back affects the thoracic spine, which affects the cervical spine, which affects the structures that feed into headache patterns. A chronic forward head posture doesn't always start in the head — it often starts with how the pelvis is tilted and how the thoracic spine compensates or even further down to the sacrum. SI joint and sciatica pain is often accompanied by headaches for that reason. Check out our post about sciatica here. Addressing headaches well sometimes means working through the whole spine, not just where the pain is felt.
What This Means for Migraine Sufferers Specifically
For patients whose migraines are triggered or worsened by physical factors — neck tension, postural strain, screen time, or the accumulated load of a demanding week — reducing that mechanical burden through osteopathic treatment can genuinely change the pattern. Not by curing the neurological component of migraine, but by raising the threshold at which triggers fire.
A patient who previously got migraines three times a month may find, after a course of treatment, that they're getting one. A patient whose migraines were severe and long-lasting may find the episodes becoming shorter and more manageable. That's not a cure — but it's a meaningful improvement in quality of life, and it's the kind of change we see regularly in clinical practice.
What we're careful not to promise is that osteopathy resolves migraines with a strong hormonal component, or purely neurological presentations where there's no meaningful structural contribution. Honesty about what manual therapy can and can't do matters — particularly for something as complex as migraine. For many frequently asked questions, visit our FAQ section for more info.
Ready to Get Your Neck Properly Assessed?
If your neck pain keeps coming back — or if it’s been quietly building and you keep putting off dealing with it — an osteopathic assessment is a practical next step. Two people can walk in with identical symptoms and have completely different underlying causes. Finding yours is what determines whether treatment actually sticks.
JD Osteopathy is located at 5025 Orbitor Drive, Building 1, Unit 101 in Mississauga, and 3141 Walkers Line in Burlington. No referral required — you can book directly online.
JD Osteopathy serves patients across Mississauga and Burlington. Our osteopathic practitioners hold a Master in the Practice of Osteopathic Manipulative Sciences (M.OMSc.) from the Canadian Academy of Osteopathy — the highest level of osteopathic education available in Ontario.
How Osteopathy Approaches Headaches and Migraines
At JD Osteopathy in Mississauga, a headache assessment looks at the whole body, not just the head and neck. We evaluate:
Upper cervical joint mobility — particularly C1 and C2, and how they're moving relative to the skull and the rest of the cervical spine
Suboccipital tissue quality — assessing tension, restriction, and asymmetry in the muscles at the base of the skull
Thoracic extension and rotation — looking at whether the mid back is contributing to cervical loading
Jaw mechanics — assessing whether TMJ restriction or clenching patterns are feeding into the presentation
Postural patterns through the whole spine — understanding the bigger picture of how the body is held
Cranial techniques where indicated — gentle work through the cranial structures to support fluid dynamics and reduce tension through the craniosacral system
Treatment is hands-on and varies significantly between patients depending on what's driving the headaches. Two people who both describe "chronic tension headaches" often need quite different approaches once assessed properly.
When to See a Doctor About Headaches
Most headaches are benign and appropriate for osteopathic assessment. However, seek immediate medical attention if you experience:
A sudden, severe headache unlike any you've had before — sometimes described as a "thunderclap"
Headache accompanied by fever, stiff neck, rash, or confusion
Headache following a head injury
Headache accompanied by neurological symptoms such as vision changes, weakness, or speech difficulty
Headache that progressively worsens over days or weeks without explanation
These require medical assessment before any manual therapy is appropriate.


